What I’ve learned about health insurance
For professional woodworkers, it pays to learn about the cost of health care before you need it.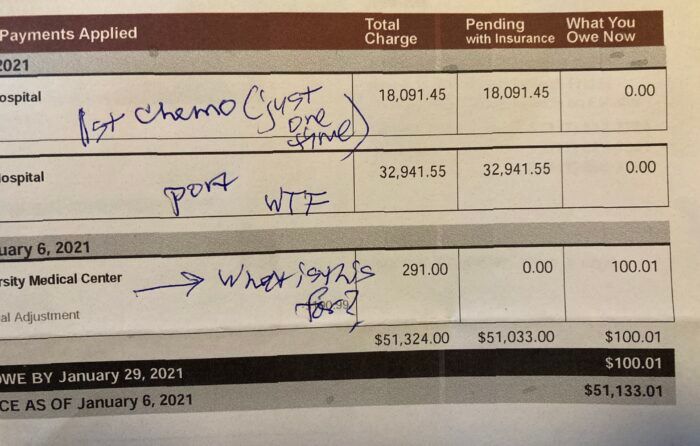
This post comes from hard-won experience – the kind from which I hope to help save you. I know a lot of self-employed people who don’t have health insurance because they say they don’t need it, can’t afford it, or it’s going to cost too much and “not pay for anything anyway.”
I get it. Health insurance premiums are expensive, especially if your household income is just high enough to disqualify you for any subsidies the Affordable Care Act (ACA) offers in an effort to make medical coverage affordable. Many woodworkers have a spouse who gets family health insurance through a group policy as a benefit related to employment. If you’re one of them, great. But if you, like my husband and me, have to go it alone, you owe it to your family and yourself to research the policies that are available and get coverage.
I have been buying health insurance since 1995, when one of my customers broke his ankle in a fall and ended up having to pay $2,000 of his $10,000 hospital bill. As a tenured professor at our state university, this customer had excellent coverage, and his premiums were enviably low. Yet he still had to pay $2,000, a sum that could easily have put my fledgling business out of commission. As soon as I heard about his plight, I contacted my insurance agent and arranged for coverage.
I was healthy and in my mid-30s at that time, so the premiums were low. (Not all states base, or based, premiums on age. Some base them on zip code and standardize rates for all.) Still, when you’re self-employed, income can be sporadic — feast or famine. At numerous times over the succeeding 25 years, paying those premiums has been a struggle. But I considered them no less important than paying my mortgage. As a professional in the building trades, I’m well aware of how easily I could be injured and rack up medical bills that might bankrupt me.
When the ACA went into force, my husband, Mark, and I weren’t even aware that there was insurance available beyond the widely publicized Marketplace plans. We discussed plans with Mark’s insurance agent (who was doing us a favor; her company doesn’t even sell health insurance any longer, but she offers assistance to clients who buy insurance of other kinds) and decided on the lowest-cost plan linked to a Health Savings Account (HSA). Even those came with a hefty price tag – in 2020, we each paid $799 a month; in 2021, it’s $845 – and it’s a plan coupled with high deductibles. When I say high deductibles, I’m talking about $7,200 per person for one recent year; this year it’s $5,400 per person. Our friend Bert Gilbert, a self-employed general contractor, calls this “don’t-lose-your-house insurance,” the idea being that you pay as little as possible in premiums, considering how expensive even the “affordable” coverage is, and when you need it, the coverage for big ticket items will be there.
Insurance is all about sharing risks, and my one-person design-build furniture business has relatively low gross revenues and profits. Like thousands of other furniture makers, I regard the satisfaction I get from work as part of my “profit,” so every year I’ve signed up for the lowest-cost HSA-linked coverage and hoped I’d never need to use it.
Then came my diagnosis of pancreatic cancer in November 2020. Cancer is one of those big-ticket items. I bided my time, waiting for bills to start coming in and realizing that neither Mark nor I fully understood our health insurance coverage. So one night, when the mail delivered a “billing statement” for $51,000 — $33,000 for my chemo port placement procedure and another $18,000 for just *one* chemo infusion – my stress level went through the roof. I knew the sums were the hospital’s raw charges – they didn’t reflect discounts negotiated by the insurance company, or any actual coverage our insurance company might pay. But even so, I knew we’d be on the hook for our deductibles, as well as the mysterious other charges that together make up our “maximum out-of-pocket expenses.”
This thing could destroy us financially. I seriously considered stopping my treatment right away, until I could get some idea of what it was going to cost. I had inquired about estimated charges before I even agreed to treatment. One oncologist told me, “No one will give you an estimate of charges.” *Friends said “do what you have to, even if you end up paying the hospital $10 a month for the rest of your life” (to which I wanted to respond with another question: If I die, does my husband then lose our house in order to pay the outstanding balance of charges? That’s not a future I want for him, and my life insurance coverage is minimal).
My cousin Gail Hiller-Lee has spent her career in the insurance industry, but I had no idea in which capacity. I contacted her and asked if we could talk. She looked at our policy and gave me the lowdown. Even at the rates we pay, we appear to be responsible for the entire “family” deductible (i.e., even though I’m the one being treated, we have to satisfy the deductibles for both of us) and maximum out-of-pocket charges, the sum of which comes to around $25,000. Gail points out that in a regular/non-HSA-compatible, fully-funded health plan plan through the Marketplace or directly through an insurance carrier, there may be two or three deductibles that each member satisfies individually. But with a high-deductible policy, deductibles are either single (for a one-person plan), or, if the plan covers more than one person, they become a full family deductible, as with ours. (More on this below.)
In our case, this $25,000 in out-of-pocket expenses will be additional to our regular business and living expenses. These charges also come in a year when neither of us will be able to do more than a fraction of our regular paid work — thanks to the pandemic, Mark is the only person I can safely be around in my immune-system-compromised state. Friends have offered to drive me to chemo, etc., but getting into a car with anyone else, no matter how safe they’ve been, is just a bad idea. Ever since March 2020, Mark has been doing fewer jobs than usual, and those have been of less-extensive scope, because he has made a point of not working around other people — for everyone’s sake. Now we’re taking that caution to even greater lengths.
And we thought we were being responsible by maintaining health insurance coverage!
Here is some extensive information and advice from Gail, along with several important definitions of terms.
First, find a broker
“There is a difference between an insurance broker and an insurance agent,” says Gail. “A broker is usually an independent adviser/salesperson who should have no allegiance to any one carrier, offering you [a choice among] everything available. An agent is an employee of a single insurance carrier and primarily sells their employer’s policies but may have the ability to sell other products, as well.”
Everyone who has a car should have a property and casualty broker, ideally someone local whom you can meet face to face, not one of those online insurance companies. When push comes to shove and you have to make a claim, having someone who knows and cares about you can make a big difference. (I know this from experience.) Does your property or business broker have someone in the office who handles health insurance? If not, see whether your life insurance agent can recommend a good health insurance broker.
You may also check with your doctor to see whether they have a broker. If not, their practice may belong to a group that does. Ask for names.
Finally, there are two associations that may be able to help you find a broker: Health Agents For America and the National Association of Health Underwriters. The latter has agents in every state. “Although HAFA has the most dedicated insurance advisers out there,” Gail adds, “they may not have someone in your area.”
Important details to be aware of
Network
Is your network local, regional, or national? If you become ill, your family is in another state, and you have to move in with them so they can care for you, it’s crucial to find out whether there’s a medical care provider there in your network. In “narrow network” plans (such as ours), there’s a local or regional network. National networks are at a premium and may or may not be available. When you’re sick and in an already-challenging situation, finding yourself seeking out-of-network care can be financially and emotionally devastating.
Determine whether your local hospital, urgent care center, and doctor are in a network before you sign up for coverage. You may get an affordable plan, only to discover that no hospital nearby is in the network – not helpful if you have a serious accident at work. While this scenario may sound unlikely, Gail has seen it happen.
Knowing your network is critical, because only charges from in-network medical providers will be covered. If you seek care at an out-of-network facility, you may find that there is no out-of-pocket limit, which can prove disastrous. And if you do have to go to the hospital, don’t just show them your health coverage card; make a point of asking “Do you participate in my insurance?” Then Gail says, “make sure that they participate in the particular network of the insurance plan you purchased.” Otherwise, you could be left with hundreds of thousands of dollars in bills that are not covered. Gail offers an example: “You call your doctor and ask if they are in Blue Cross. They say ‘Yes.’ Blue Cross has MANY networks; your doctor may take one out of the six [or however many] available. They may also say they take your insurance, but if you have both in-and out-of-network coverage, they may take your OUT-of-network portion, leaving you paying thousands before coverage even begins to pay for anything.”
Again, Gail urges, don’t just check a doctor’s or hospital’s website to see whether they participate in your network. Call the doctor or hospital and ask to make sure they are current in their network participation. Be proactive – triple-check! In some cases, even if the umbrella organization, such as a hospital, does, there may be particular departments that don’t. Even if you have a doctor who says they do participate, it’s still worth a call to confirm.
Maximum out-of-pocket expense and related terms
Among the most important innovations of the ACA are (1) an annual cap on out-of-pocket expenses, and (2) lifetime unlimited benefits. Years ago, I happened to notice that one of my policies had a maximum lifetime benefit of $1,000,000. That may sound like a lot, but if you find yourself with serious heart problems, cancer, or any number of other treatment-intensive health conditions, you can burn through a million dollars in coverage all too fast.
Calendar year or policy year
Check the wording of your policy. Any annual cap on out-of-pocket expenses will relate to one of these, but it’s important to know which one applies. A calendar year runs from January 1 to December 31; a policy year can run from the month you buy the coverage to the end of the twelfth month after. Knowing where you stand will help with financial planning.
The maximum out-of-pocket expense and the time to which it relates will have a bearing on what you have to pay. These expenses include:
- Deductibles: a negotiated figure for which you are responsible before insurance coverage will pay for certain services. For example, our plan pays for “preventive care” such as mammography and colonoscopy, but not for medical treatment per se. Some expenses are shared. With others, you have to pay for the service in full before the insurance company will begin to pay for anything else. Other plans may involve a co-pay, i.e. the patient and insurance company share the cost, and the deductible may be “waived” for doctor office visits. Also, check to see if there is a separate deductible and any limitations for drugs.
It’s important to check with your insurance company to make sure that the services you seek are “approved” and covered. If you have to pay 100% for a service, it may count toward your deductible, but not all services will. Uncovered services, which can amount to hundreds of thousands of dollars, will not count toward a deductible.
- Co-pays are negotiated, set amounts you may be charged for particular services such as doctor office visits, specialist office visits, lab and drug costs. Your policy may say you’ll pay $40 for an office visit and $70 for a visit to a specialist. The co-pay is the amount you pay your doctor at the time of your visit. The insurance carrier normally pays the rest, provided that you have met your deductible (or the deductible doesn’t apply).
You may also have co-pays after meeting your deductible. No matter what your co-pay is, it goes toward your maximum out-of-pocket expense for the policy or calendar year, depending on how your policy is worded. Note that high-deductible health plans (HDHPs) always have the deductible apply before any co-pays, but in a non-HDHP you may only have co-pays for general care and never have your deductible apply. Example: You have only office visits and drugs all year and you only have co-pays. The deductible might only apply toward advanced imaging and hospitalization, which you may not need.
- Co-insurance is a percentage you agree to pay, to share the cost of a service. For example, if you have a $1,000 deductible and co-insurance of 70%, you will pay 30% and your insurance company will pay 70%. As long as the percentage you pay for is a “covered service,” the percentage you pay in co-insurance will count toward your maximum out-of-pocket expense (also known as “maximum exposure”) for a calendar or policy year.
After you hit the maximum out-of-pocket expense, the insurance company pays 100% of all additional “approved charges” for that year, “approved charges” being those OK’d by the insurance company prior to the provision of those services.
Another important note on “policy term:” Illness and injury are no respecters of the calendar. It’s common for medical treatment to stretch from one calendar year into another. When it comes to which claims will be considered for coverage in a given year, what matters is the date of service, not when you receive the bill for that service. The charges will go toward the deductible and maximum out-of-pocket expenses for that year.
And now for some general caveats:
Explanation of benefits
Never pay a bill from anyone until you get the Explanation of Benefits (EOB) from your insurance company. If you don’t receive these in the mail, look for them at your insurance company’s website. (I found about 30 pages of these forms fully completed by the insurance company when I looked up my account online a week ago.) If a hospital or doctor sends you a bill that says you have to pay $X because your insurance company has denied the charge or hasn’t paid it, check with the insurance company. Sometimes this just means the medical service provider hasn’t yet submitted the bill to the insurance company for payment. There have been scams from hospitals and other providers of medical care in which they were paid by patients and billed the insurance company, receiving payment twice.
Pre-authorization
Many services require pre-authorization. Before you or your doctor schedules a service, make sure that it has been authorized. The doctor or hospital should obtain this authorization, but, says Gail, “you can’t count on it. Ask your health service provider to make sure that they have got the authorization, because if a doctor turns out to be out of network and did not get a service authorized, you are ultimately on the hook for those charges.” In-network doctors are responsible for obtaining this authorization, but if you show up for a test and it hasn’t been authorized by the insurance company, you’ve wasted your time – the doctor or hospital won’t complete the service without being paid. (This bit of advice comes from extended-family experience.)
Emergencies
If you have an emergency and go to an urgent care facility that happens to be outside of your network, the charges will probably not be covered.
If you go through an emergency room for emergency care, make sure they note in your file that it’s a true emergency, and it will be covered – anywhere in the country.
Prescriptions
If you use GoodRX or a similar service to get the best price on prescriptions, you need to be aware that you can either have the cost of the prescriptions covered by insurance (if it is a covered expense) or GoodRX, at least according to current law. If you go through your insurance company and the charge is a covered expense, the cost will go toward your out-of-pocket maximum. If you buy the medication through GoodRX, it won’t.
Short-term medical policies
Beware of short-term medical policies, which provide an alternative to conventional coverage or coverage in-between plans (say, if you’re changing from one job that comes with health insurance benefits to another). Some states allow these policies. Others don’t. Every one of these policies is different, and they are not subject to the ACA.
High deductible health care plans
This is what Mark and I have. First, if the policy is linked to a Health Savings Account (HSA), you have to make sure you’re actually eligible to open an HSA bank account. Not everyone is. For example, if you’re over 65 or have other insurance, such as Medicare, you won’t qualify for an HSA under IRS rules. Second, the HSA must be open before you receive medical services – until you meet your deductible, nothing besides annual preventive screenings will be covered. The least-expensive premium will likely have a high deductible (yours truly raises her hand), high out-of-pocket maximum expenses *and* the smallest network (though this last one is not necessarily the case) – in other words, the most “affordable” premium may ironically result in your biggest exposure to charges, even when you factor in the cost of your premiums.
For instance, any health plan may only cover generic drugs. In my case, our plan does not cover Neulasta, the drug used widely to stimulate the production of white blood cells in patients undergoing chemotherapy, which can make even minor infections life-threatening. Insurance companies will usually send a notice to the patient and their doctor stating that a medication is not covered. I received one of these notices about Neulasta after my oncologist ordered it. The insurance company sent a document that allowed my doctor to appeal the denial of coverage in cases where the patient’s life is at stake.
In such cases, it’s important to discuss with your doctor whether there are alternative drugs to the one denied. If not, ask your doctor for “supporting documentation” that the drug is in fact medically necessary. A doctor may also appeal a decision or have a “peer-to-peer” with the insurance carrier’s medical doctor on your behalf, to overturn a denial of any kind.
In extreme cases, your insurance broker may ask you to contact your state’s attorney general to initiate a complaint about a denial.
Finally, deductibles come in different varieties. Some are “embedded”; others are “non-embedded.” With an embedded deductible, your out-of-pocket expenses are based on each person in your family, so if only one person had expenses, they have to meet their own deductible – then the plan moves into co-insurance, etc. The family doesn’t have to reach the entire family deductible before services are paid. High-deductible plans often have non-embedded deductibles that can refer to each covered individual or the entire covered family. So in our case, we have to meet the family deductible (because there are two of us in our family, this is twice the nominal deductible, i.e. that oft-cited figure of $5,800, which we thought meant that our deductible, for each of us, would be met at $5,400), in addition to the entire family’s maximum out-of-pocket expenses, before coverage kicks in.
Marketplace versus direct carrier insurance
A few reasons why you might choose to go through the Marketplace, rather than directly to a carrier:
- Ease of all carrier information with network links available to view
- Potential subsidy, if you think you may qualify
- Information about Medicare availability
- Information regarding CHIP (Children’s Health Insurance Program)
But there are equally compelling reasons for avoiding the Martketplace:
- Employees at the Marketplace are rarely trained to help you with questions and answers about the available insurance plans
- Employees at the Marketplace rarely understand network availability
- If you qualify for just a few dollars, you’ll be required to submit quite a few tax documents — and even then, you may not know for months whether you’ve been approved. If you go directly to a carrier, you’ll have a single application, though if you apply for coverage mid-year, you may have to state a “qualifying event” in order to have your application accepted.
*Note that in many cases you can negotiate with hospitals. Tell them you have a high-deductible plan and ask if they will reduce their charges.
Finally, note that there may be changes to any of this information under the new national administration – even more reason to find yourself a trustworthy, knowledgeable broker before you buy healthcare coverage. Also, as reader Andrew Pellar pointed out, some medical costs may be deductible. Be sure to consult your tax professional.
I am deeply grateful to Gail Hiller-Lee of Bernard A. Hiller, Inc. for this crash course in health insurance.





















Comments
Oh Nancy! Wow! As a Canadian I had no idea how expensive your health insurance is!
Is there a Go Fund Me set up yet? Let’s get it going so we can help - every little bit helps and as a woodworker and a self employed person I can sympathize with the uncertainties. Please shout out if something is already set up, if not, I’ve emailed Ben Strano to see if he can help get it going.
Good of you to take the time to share all these details - I’m sure it is going to help many people.
Search on Go Fund Me for "Nancy Hiller Medical", and it should come up.
Megan Fitzpatrick set up a Go Fund me but it has since closed at Nancy's request.
Thanks! Yes, the system here is crazy. Megan Fitzpatrick at Lost Art Press organized a fundraiser that was so successful I was overwhelmed and asked her to take it offline. I appreciate your concern. So many people are in financial trouble right now thanks to fallout from the pandemic.
“[Deleted]”
Commiserations about your illness. It comes to us all, one way or another, eventually.
As a Brit I find the details of the costs involved in your treatment absolutely shocking. How can a 1st World nation have such a punitive mode of health provision in this day & age? Still, it is what it is.
As I recall, you may have British citizenship of some kind ......? If so, is return to the UK for treatment under the NHS a possibility, even in Covid times? Some 6 years ago I got Non-Hodgkins lymphoma and was treated by the local hospital for some 6 months, happily with the ideal result. It cost me nothing but the taxes I'd already paid during my working life.
Whatever you end up doing to alleviate your situation, I hope you can emerge from it all without being made a pauper by the horribly exploitative system of health "care" in the US.
Lataxe
Yes, the current US system is not conducive to sanity or financial responsibility. I'm not a Brit; I lived there for 16 years. Although I qualified for citizenship, I decided not to apply for it. We are doing our best to get through this successfully. The support and encouragement of readers and so many others have been invaluable.
I know it’s a cliché but if your advice on insurance saves one person from financial ruin due to a medical emergency, taking the valuable time to write it out was well worth it.
Best wishes to you, Nancy. The world is wonderful with you in it.
As a physician, I can verify that Nancy has given some great advice. some of the most important is to triple check coverage and to inquire if all departments in the hospital accept your coverage. Surprise Billing legislation was recently passed but may not protect all consumers. I tell my patients to "wear out" the insurance company and the hospital/doctor billing representatives with questions. If you don't have insurance, always bargain with the hospital for a cash discount. As Nancy mentions, the insurance company never pays "full price", so why should you.
Also, there is an alternative to insurance- Health Care Sharing Programs. I know several self-employed individuals that use health care sharing and have found that it is very affordable and provides excellent coverage. It is worth checking out.
I’m a retired physician, now working part-time for my wife’s mental health practice as well as doing some other stuff, unrelated to all this. My comments:
Nancy has done a superb job of describing how our “system” of health care works—or, more accurately, how we have many competing systems of health care administration (essentially, the insurers), each with multiple plans, policies, etc., which in turn contract with many competing systems of health care provision—the actual providers: doctors, nurses, other health care professionals, hospitals, etc.—that may have within them various groups that do or do not participate in the contract that the larger entity (say, the hospital) has with a given insurer. An (egregious, but realistic) example: You’re in the hospital for your hernia surgery. You checked, and the hospital and surgeon are both in-network. But...the anesthesiologist is not. Out-of-network prices in play now! And let’s suppose you have a complication of some sort, and the surgeon asks another physician to “consult” about, say, a possible infection. It is a distinct possibility that the consulting infectious disease specialist will not be in network, and the first time you learn of it is when you get the bill. (In some states, political battles are raging about how to address this, but it’s still very common in most of the country. If you don’t like it, please write your congressperson and every other person of political power you know about how unfair, costly, etc. this sort of thing is.)
Always check, if you have the opportunity, as to whether a given provider or entity is “in network”. And do it on both ends, if you can—check with the provider AND with the insurer. Sometimes the person on the phone at the hospital or doctor’s office is unaware of a change in plans, networks, or whatever, and may unintentionally give bad advice or information. Always check directly with the insurer about the network for your plan. And, like Nancy says in the article, just because a doctor’s receptionist says, “Yes, we take Blue Cross”, it does NOT necessarily mean that they are in network for YOUR plan. Example: my wife is in-network for most all Blue Cross plans, but she is not in-network for a group of plans called Blue Select; other insurers have varying networks for various groups of plans and so forth, too.
Finally, ask about plan benefits specific to the therapies, medications, etc. you expect to encounter during treatment for a given injury or illness. Mental health, for instance, is often handled much differently than many other types of care.
Most Americans end up with pretty decent medical care most of the time, in spite of—not because of—the “system” we have. Many good people work hard at providing high-quality care, but there are always some rotten apples, and any time there’s a lot of money flowing through a “system”, you can be sure that there will be innumerable administrators, managers, accountants, etc. looking for ways to funnel some of that dollar-flow toward their own or their companies’ interests.
I had surgery about 2 years ago to remove a cyst from a toe. Fairly uncomplicated stuff, for a pretty healthy guy, who more or less knows his way around hospitals and health care systems. The bill, for an outpatient procedure, totaled, before insurance adjustments, nearly $20,000. Even after the adjustments, it came to nearly $7000. I told my best friend that if I’d known it was gonna be $7K, I’d have said, “Just give me the money, and I’ll buy a couple bottles of whisky and take it out with an X-Acto knife, some scissors, and stitch it up with my wife’s sewing kit, and I’ll spend what’s left on a couple-week vacation on a beach with my foot up and a waiter bringing me drinks with little umbrellas in ‘em.”
For those who don't have a workplace insurance plan. If your gross income is not too high you could contribute to traditional IRAs to bring your adjusted gross income down to 400% of the Federal Poverty Limit in order to qualify for ACA subsidies. If it's still too high, you could put money in a 529 plan for children or some other relative. Or just donate to charity. If you can live on 200% federal poverty limit of income, and can get your adjusted gross income that low, another kind of subsidy kicks in the makes the silver plans a heck of a lot better. I think there are some situations where you can change your plan outside the enrollment period. Of course, this all depends on your State, family size, tax filing status, so on.
To add to what Nancy said about "EOB"s and bills from providers. Save those records. I have had providers come back three and five years after the mass of bills had ben settled wanting paid for something they had already ben paid for. In both cases I had changed insurance carriers and though the old carriers were helpful they were not as helpful as the one that you're paying now but I had records in hand and just needed conformation that what I was looking at was the total chargeable. Keep a record of what those old policy, group and member numbers were (I keep the old cards) so the old company can find what you need. Finally make sure your insurance is up to date. I overheard a conversation between two older fellows at a clinic twenty years ago about how much he owed the hospital. He had bought a health policy in the late fifties and a few months before the conversation had ended up in the hospital trying to find the cause of a problem he was having. After he got out of the hospital he found that his lazy agent had never up graded his coverage which had a $125,000 lifetime max. most of which he had used before he went to the hospital leaving him with $75,000 to pay on his own. He was telling his friend he could sell a parcel of property to pay the bill but the hospital had put a lien on everything he owned and wouldn't release it without payment of the bill. Also as most of you know you need a good lawyer you can trust. They can help find good agents.
Best of luck Nancy. They have made great strides in treatment of all cancers.
As a Brit with business interests in the US the contrasts between the two systems is stark. One an integrated system, free at the point of use and the other a nightmare of insurance policies. It’s not that our system is free, we pay for it through our tax system but everyone gets to access free healthcare. In general the system works remarkably well, as a company we part pay for this via what is termed National Insurance. It’s all collected via our tax system and whether you work or not you have free access to whatever healthcare you need. As a company we spend zero hours a year administering it.
I have 40 employees in CT and it seems we spend an inordinate amount of time administering the policies under what I see as a very complex system made all the more so by the whole healthcare food chain trying to make a buck.
I love the US but you should be truly ashamed of your health system.
I am so sorry to hear of your diagnosis.
I understand your frustration with our insurance industry. Why are we so opposed to a national insurance plan similar to that in Canada or England. I did not hear complaints from the Canadian or the Brit over there health care. They did comment that the pay through their TAXES, is this a dirty word. There is no free lunch!
As an older Indiana woodworker, my wife and myself, both in our eighties are now on medicare however because of the 20% deductible I carry a supplemental insurance plan. We currently spend approximately $525.00 per month for the 20% coverage to supplement our medicare with a private insurance carrier, With this coverage, and my wife has had several major surgeries, we have never spent a penny out of pocket. If the government were to "tax" or reduce our social security by this amount to have the same coverage, would this be a sin? Even with medicare the 20% can lead to finical rune for many.
Yes I am willing to contribute to a Go Fund Me to help Nancy. But what about the thousand that receive a similar diagnosis and do not have the large network of support.
I believe that if you want to help you should write your Representatives and Senators for reform of our health care system.
And yes I am still making sawdust.
Log in or create an account to post a comment.
Sign up Log in